First things first: know your fertility insurance coverage
Whether you need help understanding your fertility benefits coverage, or just want to learn about available insurance options and financial support, you’ve come to the right place.

To get started, consult with your fertility specialist
Fertility treatment costs can vary based on location, whether you’re using your own egg and sperm or not, and several other factors.
Fertility treatment costs can vary based on location, whether you’re using your own egg and sperm or not, and several other factors.
Find a fertility specialist
Use our finder tool to view different fertility clinics and help locate the right one for you.
This is not a complete list of all physicians in your area. Ferring is not responsible for the consistency and accuracy of the information provided. A listing on this site does not constitute a referral, recommendation, or endorsement for any physician or practice listed.

Next, where you live matters
Refer to the map to see what fertility insurance coverage your state offers.
As of October 2024, 22 states plus Washington, D.C. have passed fertility insurance coverage laws.
Refer to the map to see what fertility insurance coverage your state offers.
As of October 2024, 22 states plus Washington, D.C have passed fertility insurance coverage laws.

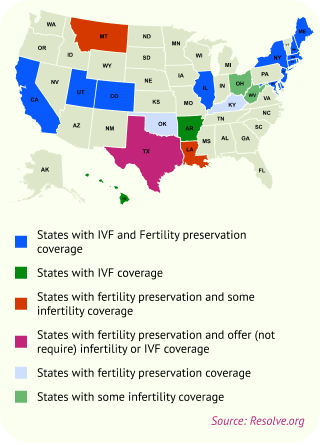
What happens if you live in one state but work in another?
Generally, the state where your employer is located determines whether or not the state mandate applies to your employer-provided health insurance plan.

Next, identify what type of health insurance you have
- Public insurance includes government programs like Veterans Administration for people who’ve served in the armed forces and TRICARE, which covers current military personnel and their families
- There are no federal mandates that require public insurance to cover infertility
Talk to your benefits provider to find out what services are covered for you
- Private insurance includes commercial insurance companies, like Aetna® and Cigna®, among others; nonprofit insurance companies, like Blue Cross®/Blue Shield®; and self-insuring groups, like employers who pay benefit claims directly instead of using an external insurance provider
- Self-insuring businesses are exempt from state mandates to provide or offer coverage. So, if your employer is self-insured, you should check with your HR representative or benefits manager to find out what’s covered for you
Ask your employer: What’s covered under my plan? What benefits do I have? How can I add benefits?
- Check to see if your fertility specialist’s practice offers cost-savings or financial programs
- Look into how you can lower your out-of-pocket costs
- Set up a meeting with your employer’s benefits coordinator or HR representative to discuss fertility treatment coverage and request changes to your plan
- Explore a variety of options beyond health insurance, like grants and scholarships, to help fund your fertility journey
For more information about insurance coverage, check out RESOLVE.org
A fertility benefits manager specializes in helping individuals access the care and support they need, with a primary focus on fertility benefits. These benefits are offered in addition to standard commercial insurance.
Providers include:
Carrot Fertility
Maven Clinic
WIN Fertility
Check out the list of terms and phrases we put together to help you speak insurance lingo.
3 tips that may help reduce out-of-pocket costs
Health insurance policies vary on how they handle coverage for fertility treatments. Your first step is to find out what your policy covers. Ultimately, it is your responsibility to know your insurance coverage, but there are places to turn for help.
If your insurance is through your work, check with your Human Resources department to speak with the person most knowledgeable about benefits. If you buy health insurance independently, ask your broker or insurance company. Most fertility clinics also have someone on staff who can help you understand your health insurance policy.
Once you understand your coverage, check out these 3 tips to help you along the way.
Many health insurance policies only pay full benefits if you use providers that are within their network. Before you start incurring costs, whether with your OBGYN or with your fertility specialist/reproductive endocrinologist (RE), confirm that the doctor you are seeing is within your network. If your doctor refers you or your partner to a specialist, first make sure that the specialist is within your insurance company’s network. Also specifically ask if all laboratories they use are in-network. This is especially the case if your fertility clinic uses an in vitro fertilization (IVF) laboratory or genetic testing service that is not a part of its clinic.
Even if your policy covers fertility, you must read the fine print to make sure that it covers the treatment and medication your doctor is prescribing. For example, your doctor might suggest that you genetically test the embryos prior to transfer to increase your odds of success. However, you might end up paying for genetic testing out of pocket, so it’s a good idea to confirm if the cost is covered first.
Another example is that your insurance may not cover all brands or types of medication. Before your treatment, let your clinic know what is covered and that you want your treatment to use the covered medication to avoid out-of-pocket costs.
Read more about insurance coverage.
Money is a valid part of deciding on a treatment plan, and your doctor should be your partner in developing an approach that will maximize your insurance coverage while avoiding as many out-of-pocket costs as possible. The following are examples of the types of things you and your doctor should consider when developing a treatment plan.
IUI requirement
Some insurance policies require a specified number of intrauterine inseminations (IUIs) before other treatments will be covered. Even if your doctor believes that IVF is your best choice for getting pregnant, your insurance may require a certain number of IUIs first before covering either.
IVF cycle limit or total dollar limit
Health insurance policies will often specify either a limit on the number of IVF cycles that will be covered or a dollar limit for all treatment. This is important information for your doctor and you to consider when creating a treatment plan to give you the best chance of a healthy baby and to avoid out-of-pocket costs.
Restrictions on coverage for some tests or procedures
Some insurance policies do not cover procedures such as intracytoplasmic sperm injection (ICSI) or assisted hatching. Knowing this in advance may alter the treatment plan.
Health insurance coverage for fertility treatments can be confusing, but with some planning, and the help of a fertility benefits manager, it is possible to maximize your coverage and avoid out-of-pocket costs on your way to having a baby.
For LGBTQ+ individuals
Building a family can be especially complex for LGBTQ+ individuals and couples facing fertility issues. These guides can help you explore your options, find affirming care, and navigate the path to parenthood with confidence.
Inclusive fertility options
Discover the different options you might hear about as you start the fertility process
Common LGBTQ+ fertility terms
Understand common LGBTQ+ treatment and testing terms you may encounter
The LGBTQ+ lawyer discussion guide
Prepare for conversations with a lawyer to ensure your parental rights are protected
A-list articles
We’ve curated our most popular articles on a range of fertility topics so you can find tips and answers, fast.
Why an OB/GYN and RE are important on your TTC team
Breaking down some common fertility traditions
How to find the right egg or sperm donor
Fertility Out Loud Docuseries
Explore the lives of four diverse couples as they navigate their fertility journeys.
Real fertility journeys
Whether you just got a diagnosis or you’ve been on the path to parenthood for some time, find strength and inspiration in other people’s experiences.
Stay informed
We’ll send you information to help you understand fertility challenges and treatment options.





